Blood vessels are far more than merely the plumbing that runs between our important organs. They’re vital in their own right, and when they’re blocked, diseased or damaged, that can cause major, sometimes life-threatening health problems. Current options for fixing or replacing them are limited, but that could be about to change (https://longevity.technology/news/novel-approach-can-engineer-blood-vessels/).
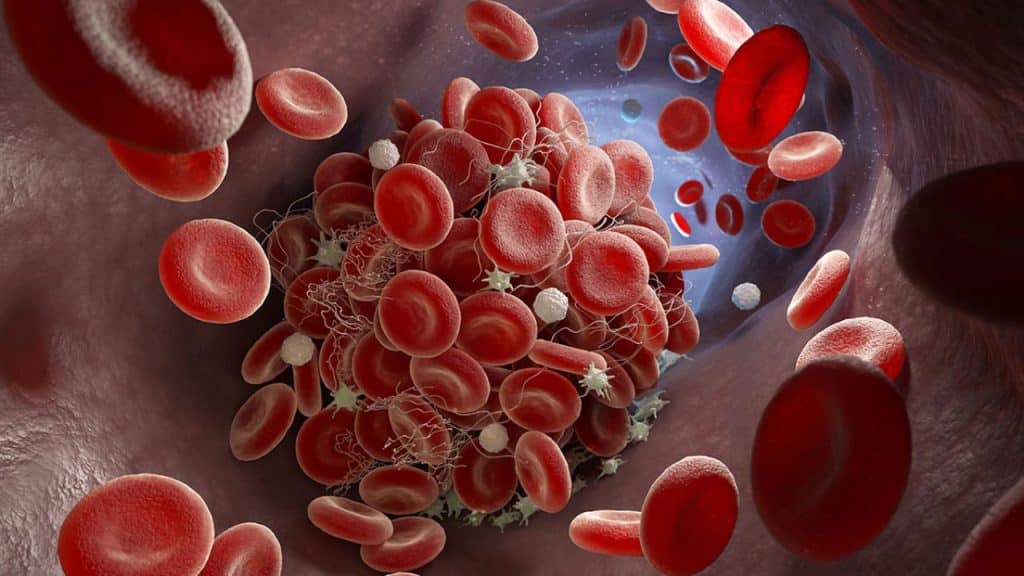
If you were to lay out your blood vessels as an adult human all in a straight line, they would span about 60,000 miles. Not all blood vessels are the same. There are arteries that take blood away from the heart and veins that carry it back again, as well as tiny little capillaries that allow various substances to transfer from blood to tissue. Their structures are similar, but their size and purpose are different.
Arteries and veins are normally constructed of three layers: a thin collection of cells on the inside, a thicker middle section of fiber and tissue, and an even more substantial layer of connective tissue, complete with its own veins and capillaries, on the outside. Capillaries only have one layer of cells, supported by a small amount of connective tissue and a thin membrane. Complex stuff.
Common issues with the blood vessels include the build-up of plaque (atherosclerosis), clots, physical damage from trauma (leading to hemorrhage) and inflammation (vasculitis). When blood can’t flow properly, nutrients don’t reach the parts of the body where they’re needed, tissue can die, and you may develop heart disease, a heart attack or a stroke. Diseases of the blood vessels are known as vascular conditions.
Currently, a common way to deal with vascular issues is through bypass. More minor blood vessels can be redirected to replace a vessel that is more important but is damaged or diseased. In other cases, synthetic grafts are used. This approach is not always effective, however, depending on the structure of the vessel that needs replacing, or the condition of the donor vessels. It’s also slow and expensive, requiring specialized equipment and difficult to perform at scale.
That’s why this new technique, developed at the University of Melbourne, is so promising. It uses human cells and live tissue to avoid the problems associated with synthetic grafts, plus a complex combination of materials and fabrication techniques. It’s faster, cheaper and if it becomes operational in bypass surgery, it has the potential to significantly improve patient outcomes.